Patient Portal
Give patients instant access to their entire clinical record via an intuitive and well-designed healthcare hub. Patient Portal seamlessly integrates with our other engagement solutions, creating a convenient and cohesive experience for patients.

.
Patient Schedule
Enable patients to quickly schedule appointments after searching and selecting a provider online, without logging into an account or downloading an app. Meanwhile, avoid unwanted overbookings and scheduling mishaps via our two-way integration with your EHR.

Patient Intake
Give patients the convenience to check in for their visit from their home, the parking lot, or your waiting room. Providers will enjoy streamlined patient processing workflows by digitizing and automating the entire intake process.

Patient Notify
Automate appointment reminders, confirmations, and organizational announcements via call, text, email, or within the Patient Portal. Maximize staff efficiency and increase practices revenues by eliminating manual patient communication workflows.

Family Portal
Empower families to manage the health of a loved one who is in long-term care, skilled nursing, and rehabilitation facilities. Family Portal offers the same easy-to-use and modern portal experience as our Patient Portal.

Patient Survey
Automatically measure patient satisfaction and capture patient-reported outcomes with completely customizable surveys. Send surveys to target populations and create automated events based on survey responses.

Patient Activate
Say goodbye to manual and inefficient population health initiatives and motivate your patients to become active participants in their own health. Automate meaningful engagement between visits using simple yet powerful tools that enable you precisely identify patients to manage, monitor, and intervene with.

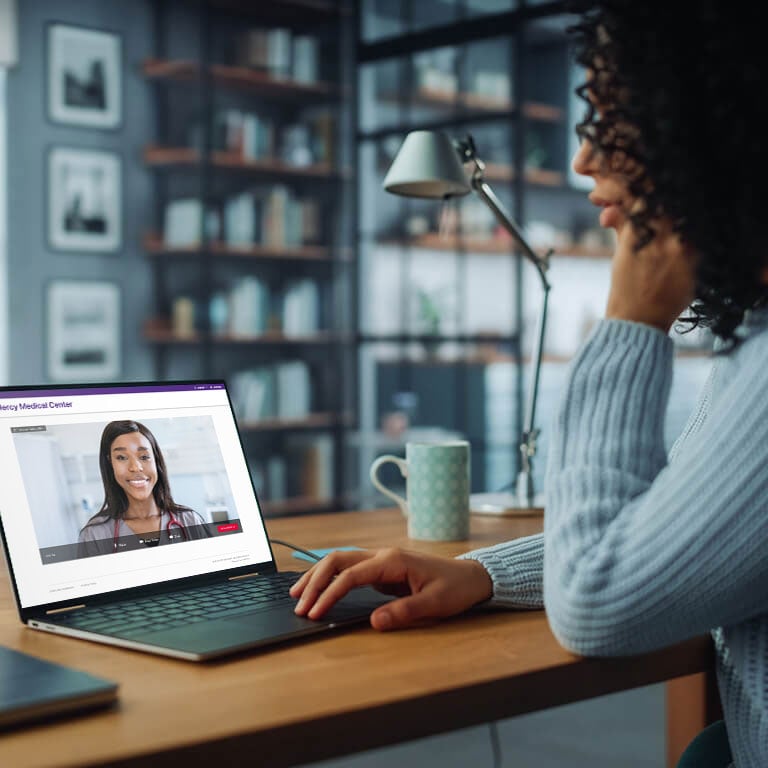
Patient eHealth
Provide a fully integrated virtual care experience that emulates a digital version of your physical practice. With options for 1:1 or group visits, providers and staff will appreciate not having to leave their current systems or workflows, while patients will love the convenience and simplicity of our telehealth solution.
 Explore Our Entire PlatformLearn more about InteliChart's Healthy Outcomes platform.Explore our individual products
Explore Our Entire PlatformLearn more about InteliChart's Healthy Outcomes platform.Explore our individual products Why Patient Engagement Requires a PlatformLearn the key solutions you need to engage patients.
Why Patient Engagement Requires a PlatformLearn the key solutions you need to engage patients.